Cataract surgery
Prof. Dr. Abela-Formanek - Ophthalmologist for ophthalmology and optometry in Vienna
Cataract surgery
Cataracts are the most common cause of visual impairment at around the age of 60.
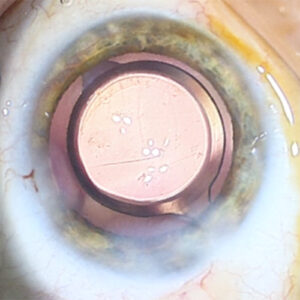
A cataract causes the lens to become cloudy when it is typically clear. Cataracts can eventually affect vision. This procedure is considered to be very common and generally safe. Nowadays, cataract surgery not only focuses on replacing the lens, but also corrects existing refractive errors, such as nearsightedness, farsightedness and astigmatism.
For a preliminary examination and planning of a cataract surgery, please make an appointment in the practice!
Focus on your eye health
Prof. Dr. Abela-Formanek looks back upon more than 25 years of experience in eye surgery and is considered an absolute expert in her field.
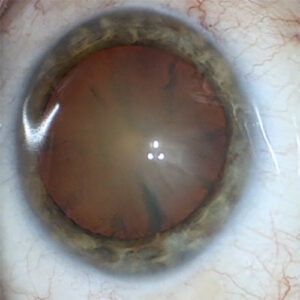
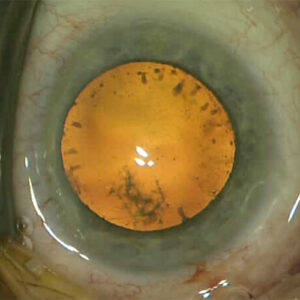
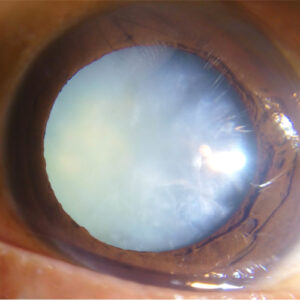
What is a cataract?
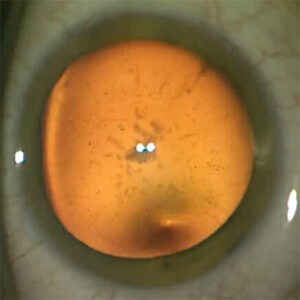
In cataracts the lens of the eye is clouded (cataracta complicata). Clouding of the human lens often develops very slowly over several years.
The causes: One of the most common causes for the development of cataracts is the natural aging process. Over the years, the metabolism of the lens slows down and as a result the lens becomes harder and loses its elasticity. Over time, vision impairment occurs due to lens opacification. Other causes for the accelerated development of a cataract can be attributed to various factors, e.g. other eye diseases (uveitis, high myopia), traumatic cataract (eye bruise, eye perforation), strong UV radiation, metabolic diseases (diabetes mellitus), chronic cortisone therapy, chemotherapy or Radiotherapy.
How do you notice cataracts yourself? Cataract symptoms develop slowly and can hinder daily activities when advanced. Below are some signs you can look out for:
- blurred vision
- glare
- Difficulty with night vision
- altered color perception
- frequent changes in glasses strength
- mono-ocular double vision
- Changes in contrast vision
The diagnosis: Progress can be determined using an eye test and an eye examination in the office. The anterior chamber, the cornea, the lens with all its layers, the vitreous body and the retina are examined. The eye is examined at the slit lamp to determine whether the lens is the only cause of the visual impairment. Precise measurements of eye length and corneal curvature are taken. An assessment is then made as to which lens should be implanted. After a consultation, it will be determined whether the operation should also correct a refractive error. After the information has been given, the patient has time to think before agreeing to an operation date and, if necessary, ordering a lens.
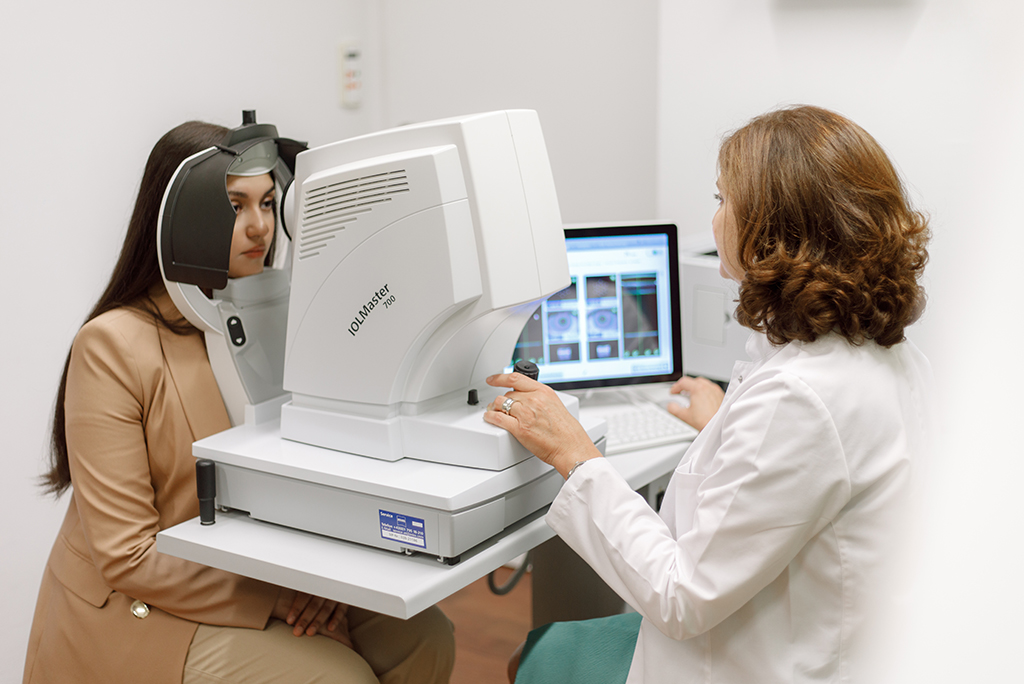
Eye length measurement before cataract surgery
IOL Master 700
This high-precision device measures the axial length of the eye, which is crucial for calculating the correct artificial lens power for cataract surgery. The measurement is non-contact and completely painless and usually takes only a few minutes.
This new device uses imaging OCT technology (SWEPT Source Biometry) and enables precise measurement of the length of the eye, even in the case of dense cataracts, including the measurement of the curvature of the cornea.
Answers to the most frequently asked questions about cataract surgery
Special lenses
Would you like to make an appointment or do you have questions about operations?
Give us a call. Dr. Abela-Formanek will be happy to answer your questions!